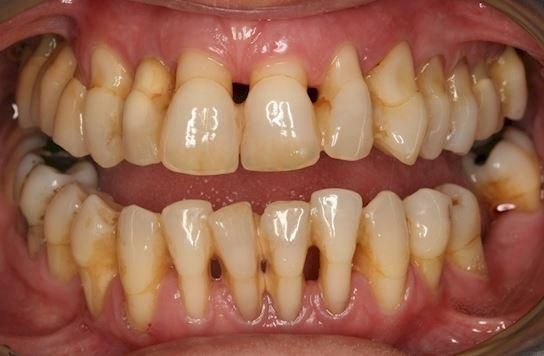
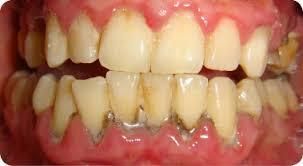
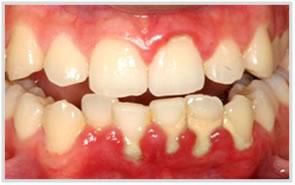
Periodontitis is a chronic, inflammatory, oral disease caused by mouth organisms (oral pathogens) resulting in destruction of the gums, connective tissue, and bone supporting the teeth. People who are at greater risk include those that neglect brushing and flossing their teeth regularly; those who use tobacco of any kind; those under stress; people with other medical diseases that lower the body’s ability to fight infections, such as diabetes or HIV; people taking medications such as steroids and blood pressure drugs; people with suppressed immune systems; those with inadequate saliva production; those with hormonal changes such as: teenagers, pregnant women, those using birth control pills; those with a family history of early tooth loss or gum disease; people who have an amplified genetic response to inflammation; and those with intimate salivary contact (the bacteria that causes gum disease is transmissible between parents and children or between couples). Periodontal disease is one of the root causes of whole body (systemic) inflammation. The disease is considered incurable, but can be successfully treated, arrested, and maintained. Warning signs may include gums that bleed when brushed or flossed; gums that are red, swollen, puffy, or tender; gums that are loose or not tightly bound to the tooth; pus or crusty deposits between teeth and gums; loose teeth; bone loss on dental radiographs; persistent bad breath; and changes in bite.
Both periodontitis and its more reversible stage, gingivitis, can result in an open wound at the junction of the gums and the tooth (gingival sulcus) which allows mouth organisms, their toxins and inflammatory contaminants to gain access to the blood stream and become metastatically transported to other organ systems. This dissemination initiates inflammatory and immunological responses both orally and systemically causing an elevation of serum pro-inflammatory chemicals, elevation in serum lipids, immunological injury, adverse organ inflammatory states, and the intravascular inflammation that promotes arterial plaque formation (atherosclerosis). Some organisms may directly invade organs, while others may damage the delicate lining of blood vessel walls, or cause bacteremia, septicemia, or endotoxemia. Other associated systemic inflammatory risks can range from an increased probability of micro-vessel dementia, retinopathy, thrombosis, impaired kidney function, pregnancy complications, insulin resistance, rheumatoid arthritis, bacterial pneumonia, digestive cancers, and vascular events linked to heart attacks and strokes.
STATISTICS:
Some type of periodontal disease or gingivitis affects 80% of the population, including 50% of American adults. Thirty percent of the population have no genetic resistance to this disease. It remains one of the most common diseases in the world, with increased rates found in lower socio-economic groups, specific races, in males, and adults over 30; it is the number one cause of tooth loss in adults. It is considered the number one oral health risk of the 21st century and is prevalent at epidemic proportions. Its progression is dependent upon the capability of the organisms to cause disease (virulence or pathogenicity), the number of pathogenic organisms involved (bio-burden), and the resistance of the host. A reduction in mouth organisms associated with periodontal infections has been shown to significantly improve systemic disease outcomes, associated complications, and related medical expenses.
PREVENTION:
- Identify specific oral pathogens and their relative amounts. Saliva testing for specific bacterial strains and quantification of pathogen levels can help dictate antibiotic therapies and reduction strategies. Certain bacterial species are known to be more aggressive and destructive to oral tissues; others have been implicated in whole body inflammation increasing risks to diabetics, heart disease patients, pregnant women, kidney disease patients, rheumatoid arthritis patients, those with lung diseases, etc.
- Improve host resistance. Treat and control systemic diseases that may lower host resistance, such as diabetes, HIV, cancer, etc. Eliminate tobacco use. Reduce stress. Genetic salivary testing can identify those people with an inherited exaggerated response to inflammation who are less resistant and at greater risk before disease appears; this information can be useful for individualized prevention planning and more aggressive interventions.
- Remove bacteria and sugar sources from the tooth surface. This is accomplished by effective and thorough brushing at least twice daily, and flossing between teeth once daily where toothbrush bristles can’t reach.
- Maintain professional dental care. Your dentist can detect gum disease in its earliest stages. Early care means treatment is simpler, quicker, less costly, conservative, and more comfortable when the disease is diagnosed and treated early. Gum disease is incurable but treatable. Crusty deposits that harbor bacterial colonies and form on the tooth and below the gum line must be removed by dental professionals in a process known as scaling and root planning. It is essential that it be maintained for the life of the dentition to control reoccurrence and minimize further damage to the gums, prevent tooth loss, and reduce damage to the bony support of teeth. Advanced disease may require referral to a gum specialist (periodontist). Dental experts can further assist on ways to be the most effective with brushing and flossing, as well as, help provide guidance on proper nutrition. Your dentist can evaluate the health conditions and medications that may contribute to gum disease progression, and advise you on the risks that gum disease poses to whole body health, oral-systemic connections. Your dentist may also prescribe antibiotics, antimicrobial mouth https://www.paperwritings.com/ rinses, and medications that may help control your inflammatory response to the disease.
Resources:

